Health
Dual Diagnosis Rehab Bakersfield: A Complete Guide to Healing Mind and Addiction Together

Dually diagnosed addiction patients have mental health issues along with their addiction and need to be specially treated. Recovering from addiction is difficult, and recovering from mental health issues along with it is even more complicated. If you are looking for dual diagnosis rehab Bakersfield, understanding the importance of this treatment could be the first step to getting better.
Having mental health issues along with addiction complicates the recovery journey. If a patient is treated for one of the issues, the likelihood of the patient relapsing is very high and the patient will just continue to suffer. This is the reason why dual diagnosis treatment is the best option for addiction recovery, and it provides patients with the support needed to fully recover.
What is Dual Diagnosis: The Intersection of Mental Health and Addiction
A dual diagnosis (co-occurring disorders) occurs when someone has both a mental health disorder and a problem with substance use. These combinations of disorders happen more often than most people think. Each year in the U.S. about 9.2 million adults report some form of mental health condition and a substance use disorder, according to the Substance Abuse and Mental Health Services Administration.
There is a complex and often two-way relationship between mental health and addiction. Some people experience mental health symptoms because of their prolonged use of a substance. Others experience the symptoms of some form of mental health disorder and use drugs/alcohol in an attempt to minimize or mask the symptoms. It does not matter if someone has a mental health disorder or substance use disorder first, both must be addressed in order to be successful in a full recovery.
Some Mental Health Disorders Frequently Seen Alongside Addiction
Many people with mental health disorders also have a substance use disorder. One of the most common is depression. People with depressive disorders often experience feelings of hopelessness, sadness, and emptiness. To escape those feelings, many people use drugs and/or alcohol. The problem with that is that substance use often leads to an increase in symptoms of depression, which creates an even more destructive cycle.
Disorders like generalized anxiety disorder, panic disorder, and social anxiety frequently co-occur with addiction. Relief from anxious thoughts with alcohol and benzodiazepines, for example, makes dependence and addiction difficult to avoid.
Another co-occurring condition is post-traumatic stress disorder (PTSD). Many trauma survivors avoid painful memories by using substances to cope. Sobriety, in this case, is unlikely without addressing trauma.
Additionally, bipolar disorder, personality disorders, attention-deficit hyperactivity disorder (ADHD), and schizophrenia are common co-occurring disorders. All are in need of integrated specialized treatment.
Why Dual Diagnosis Rehab Bakersfield Offers the Best Chance for Recovery
Integrated treatment for co-occurring disorders has the best result, compared to treatment done iteratively or one after the other. When mental illness and addiction are treated in tandem by the same specialists, the patient receives care that is specialized for the many issues that need to be tackled.
A mental health condition untreated when addiction is treated is a road to addiction relapse. Addiction untreated when mental health care is provided is a road to slow progress in therapy. Dual diagnosis care handles both at the same time in tandem.
The Integrated Treatment Approach
Dual diagnosis programs utilize an integrated method that combines mental health care with mental illness and addiction treatment with substance abuse. A single clinical team handles both problems, providing integration, collaboration, and continuity of care.
Multidisciplinary Treatment Teams
The treatment team may consist of a psychiatrist, an addiction medicine specialist, a licensed therapist, a case manager, and a co-occurring disorder treatment support staff. It makes sure that every avenue of recovery is covered.
Individualized Treatment Plans
Each recovery path is unique. Personalized treatment plans are formulated following thorough assessments and can consist of therapy, medication, group support, and holistic practices. Plans are adjusted as patients advance.
What to Expect in a Dual Diagnosis Treatment Program
Medical Detoxification
The first step of treatment for many patients is medically supervised detox, in order to ensure safe treatment of withdrawal systems. In detox, psychiatric evaluations are conducted for the identification of co-occurring disorders to begin stabilization if needed.
Individual Therapy
Patients can address the root causes of their addictions and mental health symptoms during individual counseling sessions. Some of the evidence-based methods used include:
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavior Therapy (DBT)
- Trauma-focused treatments like EMDR and prolonged exposure therapy
Group Therapy
In addition to individual therapy, group counseling offers social support and helps prevent feelings of loneliness. Group counseling can also help reinforce the skills learned in individual therapy. Some group sessions may address topics like relapse prevention, emotional self-control, communication, and other relevant themes.
Psychiatric Services
After each session, a psychiatrist may provide a diagnosis, process, and adjust medication to address symptoms, while also providing ongoing support throughout the patient’s journey.
Family Involvement in Dual Diagnosis Treatment
The entire family system is affected by addiction and mental health struggles. Effective dual diagnosis treatment programs include family therapy, support, and education to help regain trust, strengthen communication, and establish healthier family patterns.
Selecting a Dual Diagnosis Treatment Facility
Accreditation and Licensing
Confirm the treatment facility has state licensure and accreditation from recognized bodies like The Joint Commission or CARF.
Experienced Clinical Team
The staff should include licensed professionals who have dual expertise in addiction and mental health, including on the spot psychiatric support.
Proven Treatment Strategies
Therapies used should be evidence based and recognized, foregoing unproven strategies or simply desperation-based solutions.
Continuum of Care
Outpatient services, inpatient care, and long-term aftercare planning as part of the treatment process.
Location and Healing Environment
A calming and supportive space can improve engagement and increase the chances of success.
Life Post Dual Diagnosis Treatment
Aftercare Planning
Progress through therapy, psych care, and recovery tools is facilitated by structured aftercare planning.
Support Groups
Your own support is reinforced by peer programs like AA, NA, Dual Recovery Anonymous, or SMART Recovery.
Lifestyle Changes
Achieving recovery is a process of establishing healthy habits, new sober social circles, and aspirational objectives.
Ongoing Mental Health Care
Preventing relapse means staying in therapy, taking prescribed meds, and being aware of symptoms, as these are vital to maintaining your mental health.
Finding Hope and Healing in Bakersfield
With the correct assistance, it is entirely possible to recover from a co-occurring disorder. Integrated care for addiction and co-occurring mental health issues offers the greatest opportunity for successful recovery.
If you are battling mental health issues and a substance use disorder, or if someone you care for is in this situation, there is help for you. The first step toward healing is seeking help, and it is the most important thing you can do.
Bakersfield Recovery Center: Dual Diagnosis Treatment
As part of their dual diagnosis treatment program, Bakersfield Recovery Center works with the community in California’s Central Valley to combine dual treatment of addictions and disordered mental health conditions. With their trained professionals, they enforce and apply evidence-based treatment, and personalize their care strategies allowing them to assist patients in every level of their treatment and recovery process.
Health
What Your Dentist Looks for During a Routine Dental Visit
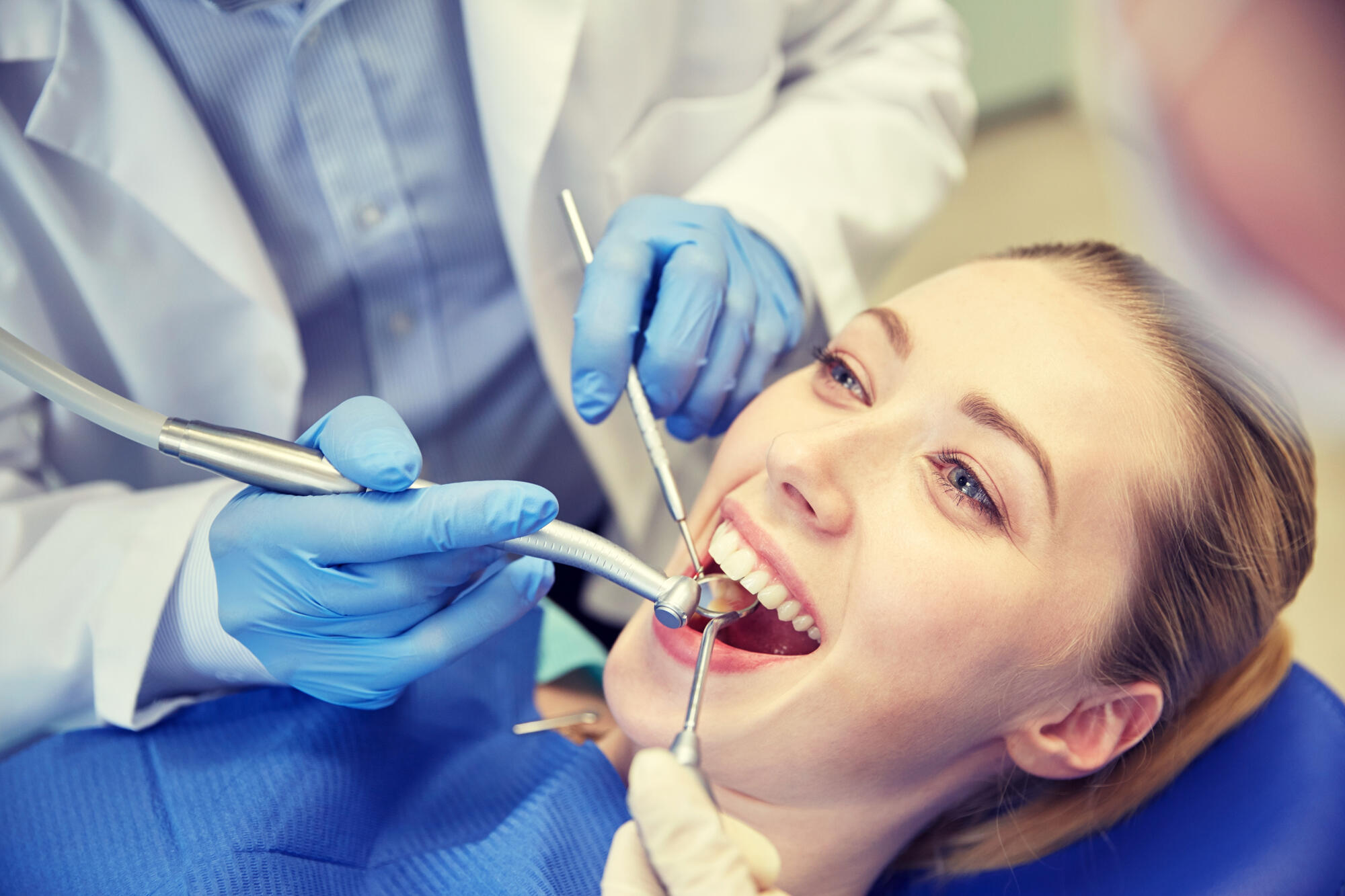
A routine dental visit may seem simple at first. Many people think it only involves cleaning teeth and checking for cavities. Yet there is much more happening during those few minutes in the dental chair. Dentists look closely at many signs that can reveal problems before they become painful or expensive to treat.
These visits are important because some dental issues do not show clear symptoms early on. A small cavity, gum problem, or bite issue may go unnoticed without a proper exam. Regular checkups help keep teeth and gums healthy while also protecting overall health.
Keep reading.
Checking Teeth for Early Signs of Damage
One of the first things a dentist checks is the condition of the teeth. They look for cavities, cracks, worn enamel, and signs of decay. Small problems are easier to fix before they turn into larger issues that may require major treatment.
Dentists also examine fillings, crowns, and other dental work to make sure they are still in good condition. Older dental restorations can wear down over time and may need repair or replacement.
X-rays may also be used during some visits. These images help dentists see areas hidden between teeth or below the gums. Problems such as impacted teeth, bone loss, or deep cavities are easier to spot with these tools.
Looking Closely at Gum Health
Healthy gums are just as important as healthy teeth. During a routine visit, the dentist checks for redness, swelling, bleeding, and gum recession. These can be early signs of gum disease.
Gum disease often begins quietly. Many people may not notice symptoms until the condition becomes serious. Early treatment can help prevent tooth loss and other complications linked to poor gum health.
An experienced dentist may also measure the spaces between the teeth and gums. Deep pockets can be a warning sign that bacteria have started damaging the tissue and bone around the teeth.
Watching for Bite and Jaw Problems
Dentists do more than examine teeth and gums. They also check how the teeth fit together when a person bites or chews. Bite problems can lead to jaw pain, headaches, tooth wear, and discomfort while eating.
Some patients grind or clench their teeth without realizing it. Signs of grinding may include worn tooth surfaces or jaw tension. Dentists often look for these clues during regular exams.
The jaw joints are also checked for clicking, stiffness, or limited movement. Small problems caught early may prevent more serious jaw issues later on.
Oral Health Can Reflect Overall Health
A dental visit can sometimes reveal signs of health conditions beyond the mouth. Dentists may notice symptoms linked to vitamin deficiencies, infections, diabetes, or other medical concerns.
The tongue, cheeks, and soft tissues inside the mouth are carefully examined for unusual spots, sores, or discoloration. Oral cancer screenings are often included in routine checkups because early detection can make treatment more effective.
These exams are one reason routine dental visits matter so much. They help protect both oral and overall health at the same time.
Routine Dental Visit: A Small Appointment With a Big Purpose
A routine dental visit involves much more than cleaning teeth. Dentists carefully look for signs of decay, gum disease, bite problems, and other health concerns that may not yet cause pain or discomfort.
Regular checkups can help prevent serious dental problems and support long-term health. Read more about how simple dental habits and regular care can protect your smile for years to come.
For more on this content, visit the rest of our blog!
Health
What Is a Bunion? Causes, Symptoms & Treatment Options
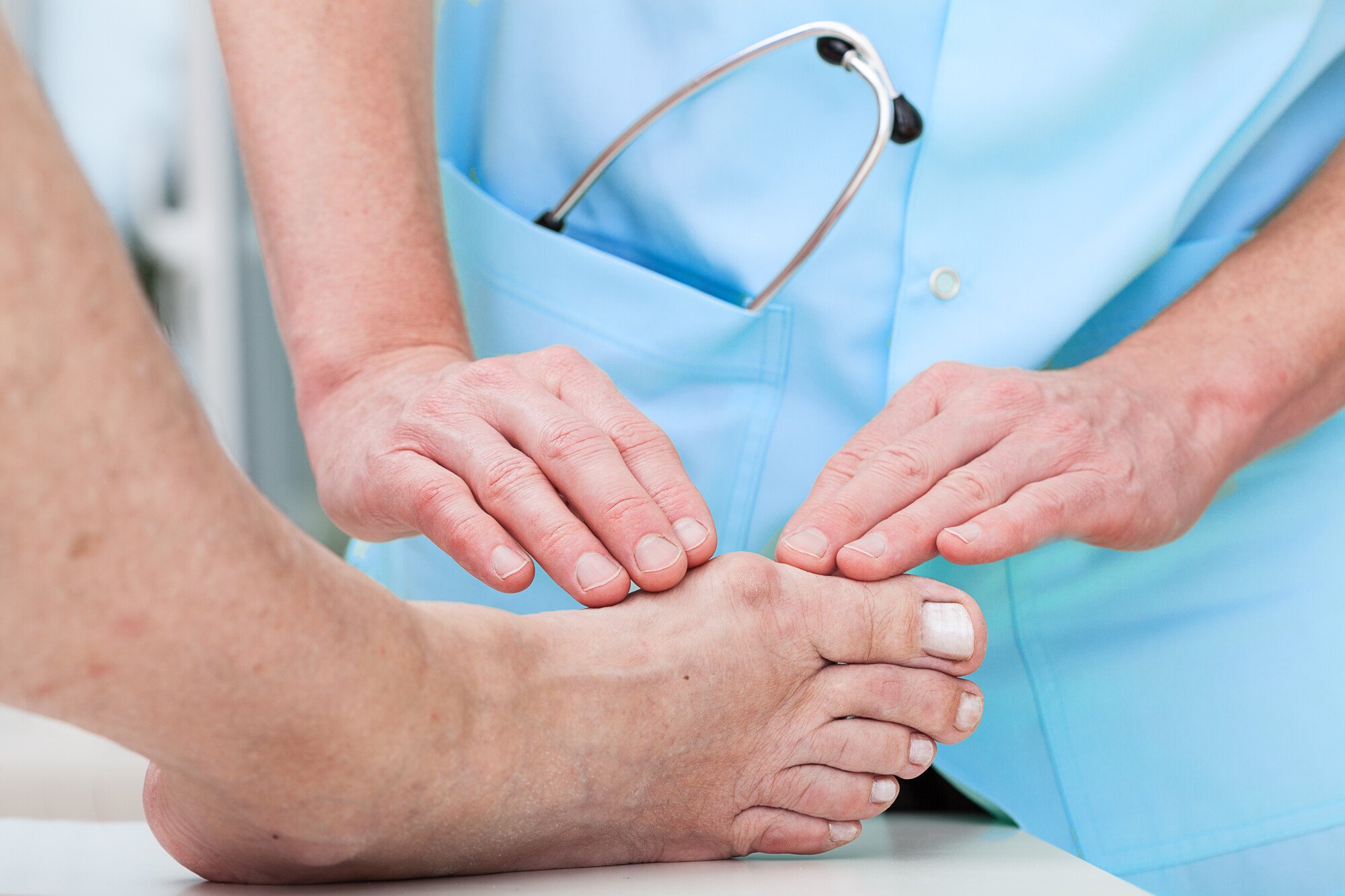
A bunion is a bump that forms near the base of the big toe. It happens when the big toe pushes against the other toes. Over time, the joint moves out of place and creates a hard bump.
Bunions can become painful and make walking harder. Bunions can happen slowly over many years. At first, the bump may seem small and painless.
As the condition gets worse, swelling and pain may appear. Continue reading to discover everything you need to know.
Common Causes of Bunions
Many bunions develop because of pressure on the foot over time. Shoes that squeeze the toes can push the big toe inward. High heels may also place extra stress on the front of the foot, and this pressure can slowly change the shape of the joint.
Some people inherit foot problems that increase the chance of bunions. Flat feet, loose joints, or unusual bone structure may lead to the condition. Arthritis can also affect the joints and make bunions more likely.
Injuries to the foot may also cause joint changes. Jobs or activities that involve standing for long hours may increase foot stress. Athletes and workers who spend many hours on their feet may notice pain sooner.
Poor foot support can make symptoms worse over time. Good footwear can help lower pressure on the joint.
Signs and Symptoms to Watch For
The most common sign of a bunion is the bump near the big toe joint. The area may become swollen, red, or sore. Some people feel pain while walking or wearing shoes, and others may notice that shoes no longer fit properly.
Bunions can also make it hard to move the big toe. The toe may become stiff and painful during movement. Corns and calluses may form where the toes rub together.
In severe cases, the toes may overlap or crowd together. Bunion surgery expert is a medical professional with advanced experience in diagnosing and treating bunions through surgical procedures that help reduce pain and improve foot function.
Treatment Options for Bunions
Many people can manage bunion pain without surgery. Wearing wider shoes helps reduce pressure on the foot. Soft pads and shoe inserts may also improve comfort.
Ice packs can help lower swelling after activity. Doctors may suggest stretching exercises to keep the foot flexible. Physical therapy may also help improve movement and reduce pain.
Anti-inflammatory medicine can help with swelling and soreness. These simple treatments often help people stay active.
Tips to Help Prevent Bunions
Wearing proper shoes is one of the best ways to help prevent bunions. Shoes should have enough room for the toes to move freely. Flat and supportive shoes place less stress on the foot.
Avoiding very tight or high-heeled shoes may help protect the joints. Keeping the feet strong and flexible may also help. Simple foot stretches can improve movement and balance.
Resting the feet after long periods of standing may reduce stress. Healthy habits can help lower pressure on the joints over time.
Living Comfortably with Bunions
Many people with bunions can still live active and comfortable lives. Early care and proper footwear often help control symptoms. Small changes in daily habits can improve foot comfort.
Regular treatment can also help prevent more serious problems. Learning about bunions can help people make better choices for foot health.
Understanding the causes, symptoms, and treatment options is important. Good prevention habits may lower the chance of future problems.
Expand your knowledge and check out more posts on our blog!
Health
Small Daily Choices That Build a Stronger, Healthier Future

Sober living is built on the small stuff Small Daily Choices.
It’s not the huge defining moments. Not the willpower. Not the quotes on your fridge. It’s the small mundane daily decisions that no one notices — the ones that you make when no one is watching. And here’s the thing…
Those small choices stack up fast.
Over the next few minutes, you’re about to discover those daily habits that really shift the needle. No fluff. All substance.
Inside this guide:
- Why Daily Choices Matter So Much In Sober Living
- The Morning Routine That Sets The Tone
- Building A Support System That Actually Shows Up
- Movement, Food, And Sleep — The Boring Trio
- Handling Triggers Before They Handle You
Why Daily Choices Matter So Much In Sober Living
Recovery is not created in a day. It’s created in the moments between the big decisions.
When you choose what to eat for breakfast. When you choose to text your sponsor instead of scroll. When you take a walk instead of sitting alone with your thoughts. Why does this matter? The brain loves repetition. Every healthy decision today makes the next one easier tomorrow.
And the data backs this up.
Data from the National Institute on Drug Abuse show that the relapse rate of substance use disorders range between 40% and 60%. That’s a frightening statistic to read at first… Until you realize that the statistic changes significantly with structure in place day to day. Successful long-term sober living often begins with one individual deciding to change one bad habit at a time. If old habits prove to be too strong of a pull, seeking professional support can help someone recover from addiction and create a new, sober routine from scratch.
The good news? After 5 years of sustained sobriety, the chances of relapsing are about 15%, on par with the general population.
That’s huge. It means consistency wins.
The Morning Routine That Sets The Tone
How you start your morning sets the tone for your entire day.
Mess up the morning and the entire day becomes more difficult. Master the morning and you’ve won before lunch. Most individuals in early recovery don’t comprehend how much havoc a botched morning wreaks.
Here’s a simple morning routine that works:
- Wake up at the same time every day — consistency trains the brain
- Drink a full glass of water before anything else — hydration matters
- Make your bed — one small win to start the day
- Move your body for 10 minutes — a walk, stretch, anything
- Write down 3 things you’re grateful for — this rewires the brain
It sounds basic, right? Well, it’s meant to. The simpler the routine, the more likely you’ll do it.
You don’t need a 2-hour ritual of green smoothies and meditation chants. You need something you can do every single day — even the bad days. Especially the bad days.
Building A Support System That Actually Shows Up
Nobody recovers alone. Not really.
Sober living is about community. The people you surround yourself with will either drag you down or pull you up. There’s no middle ground. Having a strong support system isn’t a nice to have — it’s a must have.
Your support system should include:
- A sponsor or accountability partner you can text any time
- A weekly meeting (in-person or online)
- 1-2 sober friends to call when things get hard
- A therapist or counsellor for deeper work
- Family members who understand recovery
The proof? The results of sober living homes are very impressive. The relapse rate for people who lived in one for six months or longer was just 31.6% after two years, versus 64.8% in typical aftercare.
That’s not a small difference. That’s life-changing.
Lesson? Gather your team of others on the same journey. The proper people can make recovery seem attainable — even on the darkest days.
Movement, Food, And Sleep — The Boring Trio
Want to know the most underrated tools in sober living?
Not therapy. Not journaling. Not even meetings (although those help). It’s the boring trio — movement, food and sleep. Get these right and your brain has a fighting chance to heal.
Movement
You don’t need to run a marathon. Just move every day.
A 30-minute walk. Yoga. Weights. Dancing in your kitchen. Doesn’t matter what you do. It matters that you do something. Movement pumps endorphins, reduces stress and provides you a natural high without the hangover or guilt.
Food
What you eat affects how you feel. Period.
Substances rob the body of nutrients. So healthy eating during early recovery isn’t just nice — it’s necessary. Prioritize:
- Protein at every meal — helps stabilise mood
- Whole foods over processed — less crash and burn
- Plenty of water — dehydration mimics anxiety
- Limit sugar and caffeine — both can trigger cravings
You don’t need to be perfect. Just intentional.
Sleep
This one is huge. Sleep is when your brain repairs itself.
Get between 7-9 hours a night. Go to bed the same time each night, wake the same time each morning. Turn off electronics an hour before bed.
Handling Triggers Before They Handle You
Triggers are a part of recovery. They’re not a sign of failure — they’re a sign of being human.
The aim is not to be trigger-free. The aim is to manage your triggers before they manage you.
Triggers are usually one of two things:
- External: People, places, things, situations
- Internal: Stress, anxiety, loneliness, boredom, fatigue
After identifying your triggers, you can plan to avoid them. Stay away from the people and places that tempt you. Create a “trigger response plan” so you know what to do when cravings arise.
Your plan might include:
- Calling your sponsor immediately
- Going for a walk
- Showing up to a meeting
- Using a grounding technique (5-4-3-2-1 works well)
- Removing yourself from the situation
This type of structure is important Small Daily Choices. Evidence indicates that structure and routines that support predictable daily activities correlate to a greater chance of long-term recovery success. Look ahead and your future self won’t be forced to make life and death decisions in the moment.
Bringing It All Together
Recovery isn’t made up of epiphanies. It is composed of daily decisions.
The morning you get out of bed on time. The meal you eat. The walk you take. The text you send. None of these will look impressive individually… But stack them up week after month after year — and you’ll create a life you truly love.
Quick recap of the small daily choices that matter most:
- Start your morning with a simple routine you can stick to
- Build a support system of people who pull you forward
- Move your body, eat real food, sleep properly
- Plan for triggers before they happen
Recovery is a marathon, not a sprint. The winners are the ones who keep showing up.
-

 General1 month ago
General1 month agoWhat Is Felixing? The Truth Behind a Junk Keyword
-
 Health8 months ago
Health8 months agoLufanest: Effective Local Anesthesia with Fewer Risks
-

 Entertainment1 month ago
Entertainment1 month agoهنتاوي.com: Your Gateway to Arabic Anime Content
-

 General9 months ago
General9 months agobardoek: The Artistic Heritage Inspiring Modern Creative Trends
-

 General8 months ago
General8 months agoDiscover Anonib AZN: An Anonymous Asian Forum
-

 Fashion1 month ago
Fashion1 month agoFashionisk .com Explained: A Closer Look Before You Click
-

 Lifestyle9 months ago
Lifestyle9 months agoMariano Iduba: A Visionary Leader in Global Digital Growth
-

 General1 month ago
General1 month agoWhat Is Euroyungs Com? What I Found After Digging In