Health
Building Healthy Smile Habits From a Young Age

From their first giggle to their first word, watching your child grow is a journey filled with milestones. One of the most critical—yet often overlooked—aspects of their early development is their oral health. Many parents mistakenly believe that because baby teeth eventually fall out, they don’t require the same level of vigilance as permanent teeth. However, the habits established during these formative years lay the groundwork for a lifetime of healthy smiles.
According to the Centers for Disease Control and Prevention (CDC), tooth decay remains one of the most common chronic diseases in children. The good news is that it is largely preventable. By introducing positive oral hygiene routines early, you not only protect your child’s primary teeth—which are essential for chewing, speaking, and holding space for adult teeth—but you also normalize the process of self-care. Here is a comprehensive guide to building resilient, healthy dental habits from a young age.
1. Begin Oral Care Before the First Tooth Arrives
Oral hygiene shouldn’t wait for the arrival of that first pearly white. In fact, bacteria can begin to accumulate in an infant’s mouth long before teething begins. To set the stage for good health, wipe your baby’s gums with a clean, damp washcloth or a piece of gauze after every feeding. This simple practice removes sugars from milk or formula and prevents bacteria from clinging to the gums.
Once the first tooth erupts, usually around six months of age, switch to a soft-bristled, infant-sized toothbrush. Using a smear of fluoride toothpaste no larger than a grain of rice is generally recommended by pediatric dental associations. This early introduction helps desensitize children to the sensation of having a toothbrush in their mouth, making the transition to toddler brushing much smoother.
2. Make Brushing a Bonding Activity, Not a Chore
For many toddlers and preschoolers, brushing time can become a battleground. To avoid power struggles, transform the routine into a fun, interactive event. Children learn best through mimicry, so brush your teeth alongside them to model proper technique. Show them how to brush in gentle circles, reaching the back molars and the gumline.
You can also leverage technology or entertainment to make the requisite two minutes fly by. There are numerous apps designed to gamify brushing, or you can simply play their favorite two-minute song. By associating oral hygiene with positive emotions and bonding time rather than strict discipline, children are more likely to adopt the habit willingly. Consistency is key here; doing it at the same time every morning and night cements the routine in their daily schedule.
3. Prioritize Regular Professional Checkups
Establishing a “dental home” early is vital. The American Academy of Pediatric Dentistry recommends that a child sees a dentist by their first birthday or within six months of their first tooth appearing. Early visits are less about aggressive cleaning and more about acclimatization. They allow the dentist to monitor growth and development, check for early signs of decay, and educate parents on proper care.
Finding the right provider is essential for this. You want a practice that understands the unique anxiety children may feel. For example, if you are looking for a kids dentist in South Jordan, finding a pediatric specialist who creates a welcoming environment is crucial for easing fear. A positive initial experience can prevent dental anxiety later in life, ensuring that your child views these visits as a normal, helpful part of staying healthy.
4. Rethink Snacking and Sipping Habits
Diet plays a massive role in the health of young teeth. Frequent snacking can be more damaging than the total amount of sugar consumed because it keeps the pH level in the mouth acidic for longer periods, which erodes enamel. Sticky foods like gummies, dried fruit, and even starchy crackers can cling to teeth for hours, providing a feast for cavity-causing bacteria.
Beverages are another common culprit. Putting a child to bed with a bottle of milk or juice can lead to “baby bottle tooth decay,” a condition where the liquid pools around the front teeth during sleep. Instead, encourage water as the primary thirst quencher, especially after meals, as it helps rinse away food particles and neutralizes acids. When you do offer treats, try to group them with mealtime rather than grazing throughout the day to allow saliva to do its natural protective work.
5. Master the Art of Flossing Early
Brushing alone misses about 35% to 40% of the tooth surface. Once a child’s teeth begin to touch—often around age two or three—it is time to introduce flossing. Food particles and plaque can easily get trapped in these tight spaces, leading to interproximal cavities (cavities between teeth).
Since young children lack the manual dexterity to floss effectively on their own, this will be a parent-assisted task for several years. Floss picks are often easier for parents to maneuver in small mouths compared to traditional string floss. Making this a non-negotiable part of the nightly routine ensures that as they gain coordination, they will naturally take over the task themselves without questioning its necessity.
Conclusion
Building a foundation for oral health is a marathon, not a sprint. It requires patience, consistency, and a proactive approach to hygiene and diet. By starting gum care early, making brushing enjoyable, monitoring their diet, ensuring they see a professional regularly, and introducing flossing, you are giving your child the tools they need to maintain a sparkling smile. These small daily investments yield significant long-term rewards, protecting not just their teeth, but also their overall well-being as they grow.
Health
Why Awareness-Based Movement Is the Missing Link in Modern Physical Health

Modern physical health is often associated with structured exercise routines, gym workouts, fitness challenges, and performance-based goals like strength, endurance, or weight loss. While these approaches are valuable, they often overlook a deeper and more essential layer of human movement: awareness.
Awareness-based movement focuses not just on what the body does, but on how it does it. It emphasizes sensing, noticing, and refining movement patterns so the body can function with less effort, more efficiency, and reduced pain. This is where many modern health approaches fall short—they train the body without always educating the nervous system behind the movement.
The result is that people may become stronger or fitter, yet still struggle with chronic tension, stiffness, or recurring pain. Awareness-based movement fills this gap by retraining how the brain organizes movement itself.
Understanding Awareness-Based Movement
Awareness-based movement is a practice where attention is placed on internal sensations while moving. Instead of rushing through repetitions or forcing physical effort, the focus shifts to observing:
- How movement begins and ends
- Where unnecessary tension appears
- How do different parts of the body coordinate
- Whether a movement feels easy or effortful
Over time, this awareness helps the nervous system recognize inefficient habits and replace them with more natural, balanced patterns.
Most people are unaware that a large portion of their daily movement is automatic. Sitting, standing, walking, and lifting objects—these actions are guided by learned habits that were formed years ago. Some of these habits are efficient, but many create strain without us realizing it.
Awareness-based movement brings these unconscious patterns into conscious understanding so they can be improved.
Why Modern Physical Health Is Incomplete Without Awareness
Traditional fitness systems tend to focus on external outcomes. For example:
- How much weight can be lifted
- How fast someone can run
- How many repetitions can be completed
These are measurable and useful, but they do not always reflect how efficiently or safely the body is moving.
Without awareness, the body can develop:
- Poor posture habits
- Compensatory movement patterns
- Overuse of certain muscles
- Hidden tension that leads to discomfort
This is why some people continue to experience back pain, neck stiffness, or joint issues even when they exercise regularly.
The missing link is not more exercise—it is better movement education through awareness.
The Role of the Nervous System in Movement
Movement is not just a physical action; it is a neurological process. Every time you move, your brain is coordinating thousands of signals between muscles, joints, and sensory feedback systems.
When movement is rushed or unconscious, the nervous system relies on old patterns—even if they are inefficient. Over time, these patterns become deeply ingrained.
Awareness-based movement works differently. By slowing down and paying attention, the nervous system receives clearer feedback. This allows it to:
- Identify unnecessary effort
- Reduce muscular overactivation
- Improve coordination between body parts
- Discover easier ways to perform the same action
This is why gentle, mindful movement can sometimes create more lasting change than intense physical training.
Feldenkrais Method: A Practical Approach to Awareness
One of the most well-known systems of awareness-based movement is the Feldenkrais Method. It is based on the idea that improving movement quality improves overall quality of life.
Rather than forcing correction, it uses slow, exploratory movements to help people notice how they currently move and discover alternatives that feel easier and more efficient.
A trained Feldenkrais Practitioner guides this process either through group lessons or individual hands-on sessions. The goal is not exercise performance, but learning and refinement.
People often report improvements in:
- Flexibility and mobility
- Posture and balance
- Chronic pain reduction
- Breathing and relaxation
- Overall movement comfort
What makes this approach unique is that it does not rely on physical strength. Instead, it relies on awareness and the brain’s ability to learn.
How Awareness Improves Everyday Health
When awareness becomes part of movement, even simple daily actions begin to change:
1. Sitting Becomes Easier
Instead of holding tension in the back or shoulders, people learn to distribute effort more evenly.
2. Walking Becomes Smoother
Steps become lighter and more coordinated as unnecessary effort is reduced.
3. Lifting Becomes Safer
Awareness helps prevent overuse of the back or neck by engaging the whole body.
4. Stress Decreases
Because movement and breathing are closely linked, awareness naturally supports nervous system regulation.
Over time, these small changes add up to significant improvements in comfort and physical well-being.
Why Awareness-Based Movement Is Gaining Attention
In many cities, especially wellness-focused communities like Feldenkrais Seattle, there is growing interest in movement practices that go beyond traditional exercise. People are looking for long-term solutions to pain and stress that do not rely only on medication or intense physical training.
Modern lifestyles often involve:
- Long hours at desks
- High mental stress
- Limited natural movement
- Repetitive physical patterns
These conditions create a perfect environment for tension and discomfort to develop. Awareness-based approaches offer a way to reverse these patterns gently and sustainably.
Instead of pushing the body harder, they teach the body to move smarter.
The Real Missing Link in Physical Health
The missing link in modern physical health is not strength, flexibility, or endurance. It is awareness of how movement is organized and experienced internally.
Without awareness:
- People repeat inefficient habits
- Tension accumulates unnoticed
- Pain patterns become chronic
- Movement feels effortful over time
With awareness:
- Movement becomes lighter and more efficient
- The nervous system learns new options
- Pain can gradually reduce
- Daily life feels more comfortable
This shift does not require extreme effort. It requires attention, curiosity, and the willingness to slow down enough to notice what is actually happening in the body.
Conclusion
Awareness-based movement offers a deeper understanding of physical health by connecting the body and mind through conscious attention. It reveals that many physical issues are not just structural problems, but also learned movement habits that can be changed.
Approaches like the Feldenkrais Method show that the body is capable of continuous learning and improvement at any age. Through guided exploration with a Feldenkrais Practitioner, individuals can discover more efficient, comfortable, and pain-free ways of moving.
In wellness communities such as Feldenkrais Seattle, this approach is becoming increasingly valued because it addresses what many modern systems miss: not just how the body is trained, but how it is experienced from within.
Ultimately, true physical health is not only about doing more—it is about moving with greater awareness, ease, and intelligence.
Health
Raising Awareness for the Impact of Oral Health on Vitality
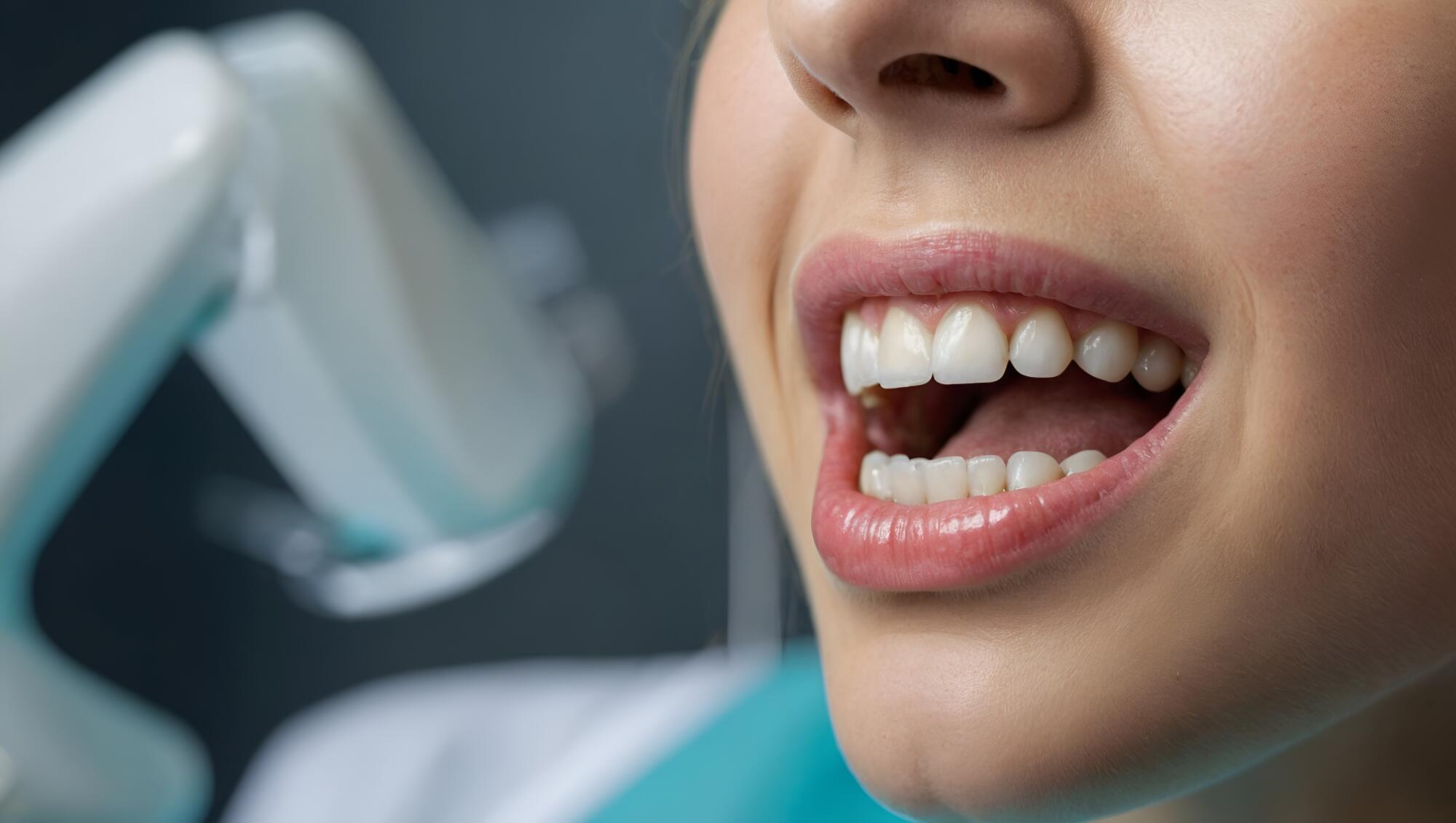
We often think of brushing our teeth as a simple daily task. It feels small and easy to forget. But oral health is more than just a bright smile. It plays a big role in how we feel every day. When our mouth is healthy, our whole body can feel better. If you want to learn how caring for your teeth can boost your energy and well-being, keep reading.
The Link Between Oral Health and the Body
The mouth is connected to the rest of the body. When there are problems in the mouth, they can spread and affect other areas. Bacteria from the gums can enter the bloodstream and travel to other parts of the body.
This can lead to issues that go beyond tooth pain. Poor oral health has been linked to heart problems, infections, and even low energy. When the body is fighting these problems, it uses more energy. This can leave you feeling tired and weak.
How Oral Health Affects Daily Energy
When your teeth and gums are not healthy, simple tasks can feel harder. Pain while eating can lead to poor nutrition. If you cannot chew well, you may avoid healthy foods.
This can affect your energy levels. The body needs proper nutrients to stay active and strong. Without them, you may feel slow and tired. There is also the stress that comes with discomfort. Ongoing pain can affect sleep and focus.
Signs You Should Not Ignore
Many people ignore early signs of oral problems. Bleeding gums, bad breath, and tooth sensitivity are often seen as minor issues. But these can be signs of deeper problems.
Headaches can also be linked to oral health. In some cases, jaw tension or dental issues may cause pain that spreads to the head. Some people even look into services like headache treatment in Woodbridge when the cause is related to oral or jaw concerns.
Paying attention to these signs can help prevent bigger problems. Early care is always better than waiting.
Building Better Oral Care Habits
Taking care of your mouth does not need to be hard. Simple habits can make a big difference. Brushing twice a day helps remove plaque and bacteria. Flossing cleans areas that a toothbrush cannot reach.
Regular dental visits are also important. A dentist can check for problems that are not easy to see. Cleanings help keep the mouth fresh and healthy.
Drinking water and eating balanced meals also support oral health. Limiting sugar helps protect teeth from decay. These small choices add up over time.
Spreading Awareness for a Healthier Life
Many people do not realize how important oral health is. Raising awareness can help change this. When people understand the link between the mouth and the body, they are more likely to take action.
Schools, clinics, and communities can play a role. Sharing simple tips and facts can help others build better habits. Education is a powerful tool for change.
When more people take care of their oral health, the result is a healthier and more active community.
A Strong Smile, A Stronger You
Caring for your mouth is a step toward a better life. It supports your energy, your comfort, and your overall health. What seems like a small habit can lead to big results.
By staying aware and taking simple actions each day, you can protect your vitality. A strong smile is more than just a look. It is a sign of a body that feels good and ready for each new day.
For more on this content, visit the rest of our blog!
Health
Chemical Peel Services for Brighter Healthier Looking Skin

Healthy skin is something many people want. Over time, skin can become dull or uneven. Sun exposure, stress, and aging can all affect how skin looks. Chemical peel services are one way to improve skin tone and texture.
These treatments help remove old skin layers. This allows fresh skin to appear. The result is often a brighter and smoother look. Continue reading to discover everything you need to know.
What Is a Chemical Peel?
A chemical peel is a skin treatment that uses a special solution. This solution gently removes the top layer of skin. It helps the skin renew itself.
As old skin peels away, new skin grows in its place. This new skin often looks fresher and more even. Chemical peels are done by trained professionals. The strength of the peel can vary based on skin needs.
Types of Skin Concerns It Helps
Chemical peels can help with many common skin issues. These include dark spots, acne marks, and uneven skin tone.
They can also help reduce fine lines and rough texture. Some people use them to improve sun-damaged skin. With regular care, skin can look smoother and more balanced.
How the Treatment Works
Before the treatment, the skin is cleaned. Then the chemical solution is applied carefully. You may feel a mild tingling or warm sensation. This is normal and usually goes away quickly.
After a few minutes, the solution is removed or neutralized. The skin then begins the healing process. Over the next few days, old skin may peel off naturally.
Medical-grade chemical peels are advanced skin treatments performed by professionals using specially formulated solutions to enhance skin texture, reduce imperfections, and promote a brighter, healthier-looking complexion under expert supervision. These treatments are stronger and designed for deeper skin concerns under professional supervision.
Different Strength Levels
Chemical peels come in light, medium, and deep levels. Light peels are gentle and have little downtime.
Medium peels go deeper and may cause more peeling. Deep peels are stronger and are used for more serious skin issues. A skin expert can help choose the right level for your needs.
What to Expect After Treatment
After a chemical peel, the skin may look red or feel sensitive. This is part of the healing process.
Peeling may start after a few days. It is important not to pick at the skin. Moisturizer and sunscreen are very important during recovery. Most people see better skin within one to two weeks.
Benefits of Chemical Peels
Chemical peels offer many benefits. They can improve skin brightness and smoothness.
They also help reduce blemishes and uneven tone. Over time, skin can look more fresh and healthy. Regular treatments can improve long-term skin quality.
Safety and Professional Care
It is important to get chemical peels from trained professionals. They know how to choose the right strength and method.
They also help reduce the risk of side effects. Following aftercare instructions is very important for safe healing. Always share your skin history before treatment.
Refresh Your Skin
Chemical peel services are a simple way to improve skin appearance. They help refresh dull skin and support a smoother texture.
With proper care and expert guidance, results can look natural and healthy. Over time, skin can feel renewed and more balanced. Taking care of your skin is a long-term process.Expand your knowledge and check out more posts on our blog!
-

 General4 weeks ago
General4 weeks agoWhat Is Felixing? The Truth Behind a Junk Keyword
-
 Health7 months ago
Health7 months agoLufanest: Effective Local Anesthesia with Fewer Risks
-

 Entertainment1 month ago
Entertainment1 month agoهنتاوي.com: Your Gateway to Arabic Anime Content
-

 General8 months ago
General8 months agobardoek: The Artistic Heritage Inspiring Modern Creative Trends
-

 General7 months ago
General7 months agoDiscover Anonib AZN: An Anonymous Asian Forum
-

 Fashion3 weeks ago
Fashion3 weeks agoFashionisk .com Explained: A Closer Look Before You Click
-

 General3 weeks ago
General3 weeks agoWhat Is Euroyungs Com? What I Found After Digging In
-

 Lifestyle9 months ago
Lifestyle9 months agoMariano Iduba: A Visionary Leader in Global Digital Growth





