Health
Adenoidid: Comprehensive Guide for Parents & Caregivers
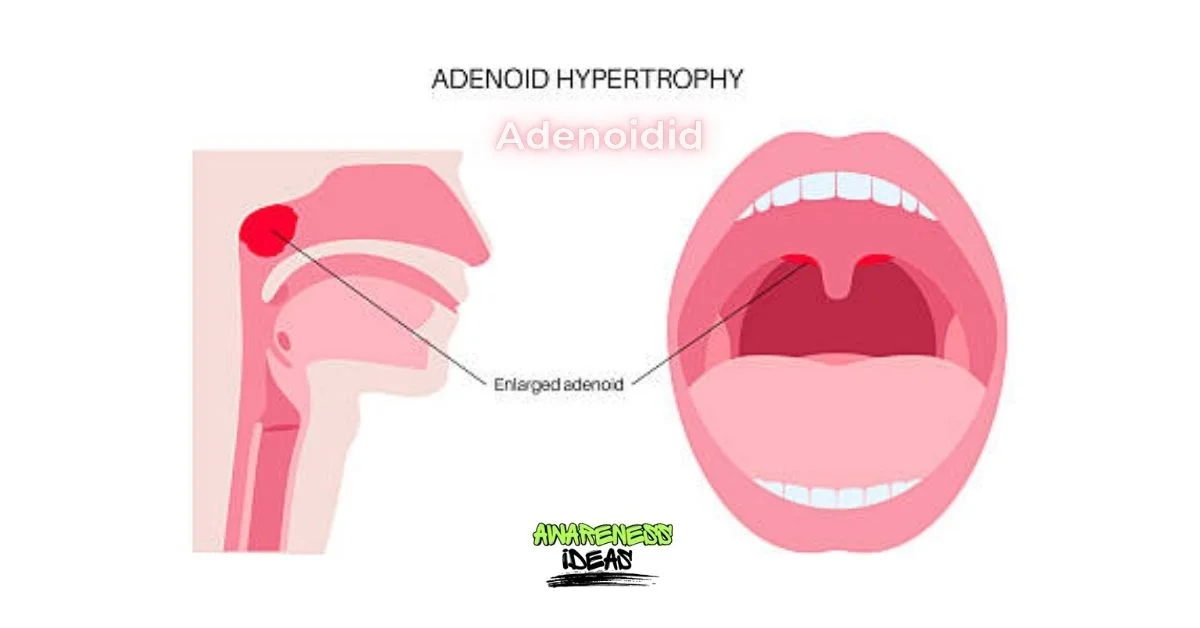
Adenoidid might not be a term that rolls off the tongue, but it’s essential for parents and caregivers to understand. These small glands play a significant role in your child’s immune system, helping to keep infections at bay. However, when adenoids become enlarged or problematic, they can lead to various health issues that affect breathing, sleep quality, and overall well-being.
As children grow and develop, their bodies go through many changes. Adenoids are part of this journey; yet many parents remain unaware of how crucial they are until complications arise. This comprehensive guide will walk you through everything you need to know about adenoidid – from what they are and why they matter to spotting symptoms early on.
Join us as we explore the world of adenoids! Whether you’re familiar with them or just starting your research out of concern for your little one’s health, this article aims to equip you with valuable insights and practical tips. Understanding these tiny glands could make a big difference in your child’s life.
Understanding Adenoids: What are They and Their Function
Adenoids are tiny clusters of lymphatic tissue found at the rear of the nasal cavity, playing a key role in a child’s immunity during early years.
These glands help trap bacteria and viruses that enter through the nose or mouth. By doing so, they prevent infections from spreading to other parts of the body.
In young children, adenoids produce antibodies that help build immunity. This is especially important as kids are often exposed to various pathogens while exploring their world.
As children grow older, adenoids typically shrink in size and may even become less active. However, for some kids, enlarged adenoids can lead to breathing difficulties or recurrent infections.
Understanding their function is key for parents looking to ensure their child’s health and well-being throughout these formative years.
Symptoms of Enlarged Adenoids in Children
Enlarged adenoids can present a range of symptoms in children that may often go unnoticed at first. One common sign is nasal congestion, which can make breathing through the nose difficult. This might lead to mouth breathing, especially during sleep.
Children with enlarged adenoids may also snore loudly or experience disrupted sleep patterns. You might notice them waking up frequently or feeling tired during the day.
Frequent ear infections are another red flag. Enlarged adenoids can block the Eustachian tubes, leading to fluid buildup and infection in the middle ear.
Additionally, some children may have trouble swallowing or complain about a sore throat regularly. It’s important for parents to be vigilant about these signs and seek medical advice when necessary.
Causes of Adenoid Problems
Adenoid problems often arise from various factors that impact a child’s health. One of the primary causes is frequent infections. Children are particularly susceptible to colds and respiratory issues, leading to inflammation in the adenoids.
Allergies also play a significant role in adenoid enlargement. Environmental triggers can cause persistent swelling, making it difficult for children to breathe comfortably through their noses.
Genetic predisposition may contribute as well. A family history of enlarged adenoids or related conditions could increase the likelihood of similar issues arising in your child.
Exposure to irritants like smoke or pollution can exacerbate symptoms too. These environmental factors aggravate existing conditions, leading to ongoing discomfort and potential complications with breathing or sleeping.
Additionally, some children may develop chronic sinusitis, further complicating their adenoid health by causing prolonged inflammation and infection.
Diagnosing Adenoid Issues
Diagnosing adenoid issues often begins with a visit to the pediatrician. The doctor will take a detailed medical history and ask about any symptoms your child might be experiencing.
A physical examination is next, usually involving looking in the throat and nose. Sometimes, doctors use special instruments to get a better view of the adenoids.
Imaging tests like X-rays or CT scans may also be recommended for more clarity on their size and condition. These tests help determine if there are any blockages or inflammation present.
If necessary, your doctor might refer you to an ear, nose, and throat specialist (ENT). This expert can provide deeper insights into potential problems related to enlarged adenoids.
Being proactive about these evaluations is crucial for ensuring your child’s overall health. Early diagnosis can lead to effective treatment options tailored specifically for their needs.
Treatment Options for Adenoiditis
When it comes to treating adenoiditis, the approach depends on the severity of the symptoms. For mild cases, doctors often recommend over-the-counter pain relievers and anti-inflammatory medications. These can help reduce discomfort and swelling.
If your child experiences frequent infections or significant breathing issues, surgical options may be considered. Adenoid removal surgery is a common procedure that can provide long-term relief. It’s typically safe and effective.
In some instances, antibiotics are prescribed if a bacterial infection is present. They can target specific pathogens causing inflammation in the adenoids.
For ongoing management, lifestyle changes such as ensuring proper hydration and maintaining good nasal hygiene can also play a crucial role in reducing flare-ups associated with adenoid problems. Regular follow-ups with healthcare professionals ensure that any treatment plan remains effective for your child’s needs.
Tips for Managing and Preventing Adenoid Problems
Maintaining good nasal hygiene is essential when managing adenoid problems. Encourage your child to blow their nose regularly, especially during cold and allergy seasons.
A healthy diet can play a significant role too. Nutrient-rich foods boost the immune system, helping fend off infections that may affect the adenoids. Include fruits and vegetables high in vitamins A and C.
Stay vigilant about allergies. Identifying and avoiding triggers, such as dust or pet dander, can minimize inflammation around the adenoids.
Promote proper hydration as well. Drinking plenty of fluids keeps mucus thin and helps prevent blockages.
Encourage regular physical activity; it supports overall health while reducing respiratory issues. Fresh air can also be beneficial for their lungs.
Make sure your child practices good oral hygiene since mouth breathing often accompanies enlarged adenoids. Regular brushing habits contribute to better overall health outcomes.
Importance of Regular Check-Ups and Consultations with a Pediatrician
Regular check-ups with a pediatrician are essential for maintaining your child’s health. These appointments provide an opportunity to monitor growth and development, ensuring that any potential issues are caught early.
During visits, doctors can assess the condition of adenoidid and other related concerns. They offer valuable insights into whether symptoms like snoring or difficulty breathing might be linked to enlarged adenoids.
Routine consultations also foster open communication between parents and healthcare professionals. This relationship enables caregivers to ask questions about their child’s health needs without hesitation.
Moreover, preventive care is vital. Vaccinations during these visits help protect children from various illnesses that could further complicate existing conditions like adenoiditis.
By prioritizing regular check-ups, you’re actively participating in your child’s overall well-being and setting the stage for a healthier future.
The Role of Parents and Caregivers in Caring for Children with Adenoidid
Parents and caregivers play a crucial role in managing adenoidid in children. They are the first line of defense when it comes to recognizing symptoms early on. Being aware of changes in breathing patterns, sleep disturbances, or frequent ear infections can lead to prompt medical attention.
Communication with healthcare providers is essential. Parents should feel empowered to ask questions and express concerns during visits. Keeping track of any recurring issues can provide valuable information for pediatricians.
Encouraging healthy habits at home also makes a difference. A balanced diet supports immune function, while proper hydration aids overall health. Creating an environment free from allergens helps reduce irritation linked to adenoid problems.
Emotional support cannot be overlooked either. Children may feel anxious about medical appointments or treatments, so reassurance and understanding go a long way in easing their fears and fostering resilience through challenging times.
Conclusion
Adenoidid, while often overlooked, plays a significant role in our children’s health. Understanding what adenoids are and how they function can empower parents and caregivers to advocate for their child’s well-being. Recognizing the symptoms of enlarged adenoids is crucial for timely intervention.
Awareness of potential causes behind adenoid issues can help in identifying problems early on. Proper diagnosis through medical consultation ensures that children receive the care they need without unnecessary delays or complications. Treatment options vary but can provide relief from discomfort and prevent future complications.
Managing and preventing adenoid problems involves maintaining good hygiene practices, monitoring allergies, and ensuring regular pediatric check-ups. Parents play a vital role in this journey by staying informed about their child’s health needs.
Caring for children with concerns related to their adenoids requires vigilance, communication with healthcare providers, and proactive management strategies. By taking these steps together as a team—parents, caregivers, and medical professionals—we can ensure healthier outcomes for our little ones as they grow.
Health
The Importance Of Transitional Care From Baby Teeth To Permanent Smiles

You might be watching your child wiggle that first loose baby tooth and feeling a strange mix of excitement and worry. It is a big milestone, yet in the back of your mind, you may be wondering whether everything is developing the way it should, if there will be crowding, or if a cavity today might affect your child’s adult teeth tomorrow. A visit to a family dentist in South Lake Tahoe can help answer these concerns. Because of this tension, it is easy to feel a bit overwhelmed and to hope things will simply “work themselves out.”
That reaction is completely human. Childhood already moves fast enough. Still, this period when baby teeth give way to permanent teeth is not just a cute photo moment. It is a window of time when small choices have long-lasting effects on your child’s future smile, comfort, and confidence. Transitional care is about guiding your child from baby teeth to a healthy permanent smile with as few surprises as possible. It means understanding what is normal, what is not, and how a trusted family dentist can help protect those new teeth before problems grow expensive or painful.
In simple terms, here is the big picture. Baby teeth hold space, guide jaw growth, and affect speech and eating. Permanent teeth arrive in stages and are more vulnerable than many parents realize in the first few years after they erupt. Thoughtful care during this “in between” phase lowers the risk of cavities, crowding, and emergency visits later. With a bit of planning and support, you can move from worry to a calm, steady plan for your child’s oral health.
What is really happening when baby teeth make way for adult teeth?
On the surface, it just looks like wiggly teeth, tooth fairy visits, and maybe a gap-toothed smile in school pictures. Under the gums, though, a lot is going on. Baby teeth are loosening because the roots are being absorbed as the permanent teeth push upward. The jaw is growing. New molars are coming in behind the baby teeth, even before all the baby teeth have fallen out.
If you have ever wondered whether your child’s timing is “normal,” you are not alone. Many parents compare their child to classmates and worry if the child’s teeth fall out too early or seem to fall out too late. In reality, there is a wide normal range. Resources such as this tooth development guide from MedlinePlus show typical ages for each tooth, which can be reassuring. Still, charts are only a starting point. Your child’s unique growth, habits, and health history also matter.
Because of all these moving pieces, this transition period is when a family dentist can spot early warning signs. For example, a baby tooth that stays in place long after the adult tooth is ready can cause the permanent tooth to erupt in the wrong position. Teeth that arrive very crowded can raise the risk of cavities and gum problems. When no one is tracking this process, small red flags can go unnoticed until they are much harder and more expensive to fix.
Why can this transition feel so stressful for parents?
The stress usually comes from three places. There is the emotional side, where you want to protect your child from pain or teasing. There is the practical side, where you worry about the cost of orthodontics or fillings. And there is the uncertainty, where you are not sure what is “worth” addressing early and what will correct itself over time.
Consider a common “what if.” A seven-year-old has several cavities in baby molars. It is tempting to think, “They are going to fall out anyway, so why spend money fixing them?” The problem is that those baby molars often stay in place until age ten to twelve. If they become infected, the pain, missed school, and possible emergency treatment can be far more draining than basic fillings. On top of that, losing them too early can cause nearby teeth to drift, stealing space from the permanent teeth and increasing the chance of braces later.
Another scenario. A child’s front permanent teeth come in with small grooves or pits. They look a bit uneven or rough. It might not seem urgent, yet these tiny grooves can trap plaque and lead to early decay. Protecting these areas with tools like dental sealants can change the whole story. The CDC explains how sealants can greatly reduce cavities, especially in children’s molars. Without that knowledge, a parent might miss a simple way to protect their child’s new teeth during the most cavity-prone years.
So, where does that leave you? Caught between “I do not want to overreact” and “I do not want to regret waiting.” That is where thoughtful transitional care and a steady family dental care plan come in. The goal is not perfection. It is early, reasonable prevention and guidance, so you are not left scrambling when something hurts or looks crooked.
How does a family dentist guide this change from baby teeth to permanent teeth?
A family dentist who follows your child over time does much more than count teeth. Regular visits in this phase are about tracking growth, timing, and habits, and then making small adjustments that protect the future smile. This includes checking whether baby teeth are falling out in a healthy order, watching how permanent teeth erupt, and spotting crowding or bite issues early.
Visual tools help too. Many dentists use growth charts, photos, or X-rays to show parents how the roots of baby teeth are shortening and how the permanent teeth are lined up beneath the gums. If you are curious about what is happening under the surface, you can look at images similar to this eruption pattern illustration from MedlinePlus. Seeing the “why” often makes treatment decisions feel less mysterious.
Transitional care also focuses on protecting new enamel. Freshly erupted teeth, especially the first and second permanent molars, are more vulnerable to decay. Sealants, fluoride treatments, and guidance about brushing and diet can make a big difference right when those teeth are most at risk. In many cases, a short, simple preventive visit today can prevent a painful filling or even a baby root canal in the future.
What are the tradeoffs of “wait and see” versus proactive transitional care?
Parents often weigh two paths. Do you wait and hope that teeth straighten out and small problems stay small, or do you act early and wonder if you are doing too much? A clear comparison can help you decide what feels right for your family.
| Approach | Short-term impact | Long-term impact | Common outcomes |
| “Wait and see” with minimal checkups | Less time in the dental chair. Lower immediate costs. | Higher chance of hidden decay, crowding, or bite issues that need bigger treatments later. | More emergency visits. Higher likelihood of extractions, extensive fillings, and complex orthodontics. |
| Proactive transitional care with a family dentist | Regular checkups and preventive visits. Modest, predictable costs. | Better chance of catching issues early while they are easier and less costly to fix. | Fewer surprises. More comfortable visits. Greater chance of a stable, healthy adult smile. |
No path is perfect. Life happens. Yet when you understand these tradeoffs, you can choose from a place of clarity instead of fear. Transitional care is not about doing every possible treatment. It is about regular oversight and a few well-chosen preventive steps that protect the emerging adult teeth.
What can you do right now to protect your child’s permanent smile?
1. Schedule consistent checkups during the “mixed dentition” years
The mixed dentition phase is when your child has both baby and adult teeth, usually from about age six to twelve. During these years, try not to skip routine visits, even if nothing seems wrong. At each visit, ask your dentist specific questions, such as which teeth are expected to come in next, whether there are any early signs of crowding, and what they see as the biggest risk for your child right now, such as cavities or habits like thumb sucking or teeth grinding.
2. Focus on prevention where it matters most
Talk with your dentist about targeted prevention for the new permanent teeth. Ask whether sealants are recommended for your child’s molars and what type of fluoride is best at home and in the office. Review your child’s brushing technique together. New molars sit far back in the mouth, so children often miss them. Simple daily routines, like supervised brushing before bed and limiting sticky snacks, protect both baby teeth and the new adult teeth that are just coming in.
3. Watch for small signs and speak up early
You see your child more than anyone else. If you notice mouth breathing, snoring, frequent mouth pain, or teeth that look very crowded or crooked as they erupt, bring it up at the next visit instead of waiting. Sometimes a small intervention, like a space maintainer after a baby tooth is lost too early, can prevent much bigger orthodontic issues later. Early conversations with your dentist help you map out possible orthodontic needs gradually instead of facing them as a sudden surprise.
Moving from worry to a confident plan
The shift from baby teeth to adult teeth is not something you need to manage alone. You do not have to know all the timing charts or predict which tooth will appear next. What matters is that you stay engaged, ask questions, and partner with a trusted family dentist who understands this transition and respects your concerns and budget.
Your child’s smile does not need to be flawless. It needs to be healthy, comfortable, and strong enough to carry them through the rest of their life. Thoughtful transitional dental care during these in-between years is one of the quiet ways you can give them that gift. You already care enough to be reading and wondering. The next step is simple. Keep the conversation going with your dentist, and use this season of change to build the foundation for a lasting, confident smile.
Health
How Fitness Drinks Supply Supports Gyms and Wellness Centers

Gyms and wellness centers do more than provide exercise equipment and training programs. They also help members stay refreshed and energized before, during, and after workouts. A reliable fitness drinks supply can support these goals while improving the overall member experience.
Offering the right beverages can add value to any fitness facility. From hydration support to convenient drink options, these products help members stay focused on their health goals. Here’s how fitness drinks supply benefits to gyms and wellness centers.
Read on!
Providing Hydration for Members
Water loss happens naturally during exercise. When people sweat, their bodies need fluids to maintain performance and comfort. Fitness drinks give members a convenient way to replace lost fluids.
Many gyms stock beverages that focus on providing hydration for active individuals. Easy access to these drinks encourages members to drink more often. This helps them feel better throughout their workouts.
Supports Recovery After Exercise
After intense training sessions, the body needs nutrients and fluids to recover. Many fitness beverages contain ingredients that support muscle recovery and energy restoration. These drinks can be useful for members with active lifestyles.
Offering recovery-focused beverages gives members more choices after their workouts. It also helps gyms meet the needs of people with different fitness goals. This added convenience can improve the overall gym experience.
Offers Solutions for Different Fitness Goals
Not every gym member has the same needs. Some people want low-calorie drinks, while others prefer protein-rich beverages. A varied drink selection helps serve a wider range of customers.
By offering multiple options, gyms can better support beginners and experienced athletes alike. Members appreciate having products that match their personal preferences. This can make a fitness facility more appealing.
Helps Prevent Common Hydration Issues
Long workouts and intense training sessions can lead to fluid loss. In some cases, this may contribute to an electrolyte imbalance that affects physical performance. Fitness drinks can help support proper fluid and mineral intake.
Providing suitable beverage options allows members to replenish what they lose during exercise. This can help them maintain comfort and energy levels. Access to these products adds practical value to gym services.
Creates Additional Revenue Opportunities
Fitness drinks can become a valuable source of extra income for gyms and wellness centers. Members often prefer buying refreshments on-site rather than bringing them from home. This creates a simple retail opportunity.
Working with a trusted gym drinks supplier can help facilities maintain a steady inventory. Reliable stock levels ensure popular products remain available. This supports both member convenience and business growth.
Improves the Overall Member Experience
Members appreciate services that make their visits easier and more enjoyable. Having access to healthy hydration choices can contribute to a positive workout environment. Small conveniences often make a lasting impression.
A well-planned beverage program can lead to enhanced member satisfaction over time. People are more likely to return when their needs are consistently met. This can strengthen loyalty and support long-term membership retention.
Boosting Revenue and Wellness With a Reliable Fitness Drink Supply
Fitness drinks supply plays an important role in modern gyms and wellness centers. It helps support hydration, recovery options, and convenience for members with different goals. These benefits can improve both member experiences and facility operations.
By offering quality beverage choices, fitness facilities can better serve their communities. Members gain access to healthy hydration solutions that fit their active lifestyles. At the same time, gyms can create added value and encourage long-term engagement.
Did you find this article helpful? Visit more of our blogs.
Health
Why Preventive Dentistry Matters For Cosmetic Success At Any Age

You might be feeling a mix of frustration and hope right now. Maybe you are noticing stains in every photo, small chips that seem to catch the light the wrong way, or gums that do not look as healthy as they once did. A Midlothian TX dentist can help you address these concerns. You want a smile that feels like you, only brighter and more confident, yet you may also worry about cost, discomfort, or whether you are “too late” to really change anything.end
At the same time, you might sense that simply whitening your teeth or getting a quick cosmetic fix will not address the deeper issues. You may be asking yourself whether your mouth is actually healthy enough for cosmetic work, and what could go wrong if it is not. That concern is wise. The truth is simple. Beautiful cosmetic results depend on quiet, steady preventive care underneath. When prevention is strong, cosmetic dentistry tends to last longer, feel better, and look more natural at any age.
So the core idea is this. If you want a smile that looks good and stays that way, prevention is not extra. It is the foundation. Once that foundation is solid, cosmetic treatments can be safer, more predictable, and often more affordable over time.
Why a “perfect” smile can still feel wrong if prevention is missing
Imagine you invest in whitening, veneers, or bonding and you love the result at first. The color is right, your teeth look straighter, and you finally feel comfortable smiling. Then a few months later, your gums start to bleed when you brush. Cold drinks sting. A small dark line appears at the edge of a crown. Suddenly the smile that was supposed to boost your confidence is causing more stress than before.
This is the gap many people fall into. Cosmetic treatments can cover discoloration, chips, spacing, and worn edges. They cannot fix untreated decay, gum disease, clenching, or poor home care. Those issues quietly continue under the surface. According to the Centers for Disease Control and Prevention, tooth decay and gum disease are still among the most common chronic conditions in the United States. That means a lot of people are asking for cosmetic care while carrying active disease they may not even feel yet.
Because of this tension, you might wonder if it is risky to pursue cosmetic dentistry when your mouth is not perfectly healthy. The honest answer is that it can be. For example, placing veneers on teeth with untreated decay can trap bacteria, leading to larger cavities and possible root canal treatment later. Whitening teeth with active gum disease can increase sensitivity and irritation. Even something as simple as bonding can fail early if your bite is not balanced or you grind your teeth at night.
On the emotional side, this can be draining. You invest time, money, and trust. You want to feel done for a while. Instead, you may find yourself back in the dental chair for repairs, touch ups, or more involved treatment. It can feel as if you are chasing a moving target.
So where does preventive dentistry fit into cosmetic success?
Preventive care is often thought of as “just cleanings” or “just checkups,” but it is much more than that. It is the quiet work of keeping your teeth, gums, and supporting bone stable so that any cosmetic care has a strong base to rest on. When you focus on preventive care for a beautiful smile, you are not only avoiding problems. You are actively protecting the cosmetic work you either already have or are planning to get.
Preventive visits allow your dentist to detect small issues before they become big ones. A tiny cavity can be treated with a small filling instead of later requiring a crown. Mild gum inflammation can be reversed with better home care and professional cleaning instead of progressing to bone loss. Research summarized in the NCBI oral health resource shows that early detection and intervention significantly reduce the severity and cost of dental disease over time.
This matters for cosmetic success at any age. If you are younger, prevention can delay or reduce the need for major cosmetic work, and when you do choose it, your teeth are stronger. If you are older, prevention helps protect existing restorations, manage dry mouth or medication effects, and keep your gums healthy enough to support cosmetic improvements. There is no age at which preventive care stops paying off.
What happens when you compare “quick fix” cosmetic care to prevention first?
You might be weighing your options right now. Do you go straight for whitening, veneers, or bonding, or do you slow down and address preventive needs first. The answer often comes down to how long you want your results to last and how much stress you want in the process.
The value of preventive care before cosmetic work is not just a theory. Dental schools and public health experts consistently highlight it. For example, the University of Illinois Chicago describes the long term value of preventive visits for both health and cost in its discussion of the value of preventive oral health care. When prevention is in place, you tend to need fewer emergencies and fewer large, urgent procedures.
The comparison below can help you see the tradeoffs more clearly.
| Approach | Short term experience | Long term impact on your smile | Typical risks | Financial picture over time |
|---|---|---|---|---|
| Quick cosmetic fix without prevention | Fast visible change. Whitening, bonding, or veneers done with minimal prep work. | Results may fade or fail sooner. Higher chance of sensitivity, gum issues, or hidden decay spreading. | Breakage, staining at edges, gum recession around restorations, need for retreatment or more complex procedures. | Lower upfront cost in some cases, but higher chance of future repairs and unplanned expenses. |
| Prevention first, then cosmetic care | Slightly slower process. Checkups, cleanings, and needed repairs before cosmetic steps. | Cosmetic work tends to last longer, feel more comfortable, and look more natural over time. | Fewer complications. Problems are usually smaller and easier to fix if they appear. | More planned and predictable costs. Often lower lifetime spending because major crises are avoided. |
| Ongoing preventive care with existing cosmetic work | Regular visits. Professional cleaning around veneers, crowns, and fillings. Bite checks. | Restorations stay brighter and more stable. Gums remain healthier which improves overall appearance. | Reduced risk of decay under crowns or veneers and less chance of sudden cosmetic failure. | Helps protect the investment you have already made. Spreads costs out with routine care instead of emergencies. |
How can you use prevention to protect and enhance cosmetic results?
So, where does that leave you. It means you have more control than you may think. You do not have to choose between health and appearance. You can build a plan that respects both. Whether you are considering teeth whitening, bonding, veneers, or a full smile makeover, you can start by strengthening the health of your mouth so your cosmetic results have every chance to succeed.
Here are three practical steps you can take right away.
1. Ask for a “health first” cosmetic consultation
When you meet with a general and cosmetic dentist, be clear that you want your mouth thoroughly checked before any cosmetic work begins. Ask them to walk you through your current situation. Which teeth are strong. Where is there early wear, recession, or decay. How healthy are your gums. A general and cosmetic dentist who values prevention will welcome these questions.
Request that your plan put disease control, gum health, and bite stability first. That may mean treating small cavities, adjusting your bite, or improving home care before whitening or placing veneers. It can feel like a slower start. It is actually what allows your future cosmetic results to last longer and feel more natural.
2. Strengthen your daily routine with small, consistent habits
Cosmetic success is not only about what happens in the dental chair. It is also about what happens in your bathroom mirror twice a day. Focus on brushing gently for two full minutes with a fluoride toothpaste, flossing or using interdental cleaners once a day, and limiting frequent snacking on sugary or acidic foods. These simple habits help prevent new decay and gum inflammation that could threaten your cosmetic work.
If you already have restorations, pay special attention to the edges where teeth meet veneers, crowns, or fillings. Those areas can collect plaque more easily. Ask your dentist or hygienist to show you how to clean around them. These extra few minutes each day are a direct investment in the life of your cosmetic treatment and your overall oral health.
3. Commit to regular preventive visits as “insurance” for your smile
Think of your checkups and cleanings as a maintenance schedule for your smile. Regular visits allow your dentist to spot early changes in your gums, enamel, and restorations long before you feel pain or see visible damage. This is especially important after whitening, bonding, or veneer placement. Small adjustments or cleanings at the right time can prevent chipping, staining, or gum irritation from turning into larger problems.
Even if you have gone years without consistent care, you can start now. There is no expiration date on improving prevention. When you commit to ongoing visits, you give yourself the chance to keep any cosmetic work you choose looking fresh and feeling comfortable for many years.
Bringing it all together for a confident, healthy smile at any age
You may have started this journey thinking mostly about color, shape, or alignment. Those things matter. They affect how you feel when you meet someone new, sit in a meeting, or pose for a photo. Yet beneath every bright, confident smile that lasts, there is quiet preventive care doing its steady work. When you honor that connection between prevention and cosmetic dental care, you give yourself the best chance at results that are not only beautiful but durable and comfortable.
Whether you are considering a small change or a full transformation, you are not behind and you are not asking for too much. You are simply looking for a smile that matches who you are. Start by making prevention your ally. Ask thoughtful questions, seek a general and cosmetic dentist who values long term health, and build a plan that protects both your appearance and your wellbeing.
Cosmetic success at any age is possible when prevention comes first. Your next step can be as simple as scheduling a preventive visit, having an honest conversation about your goals, and choosing care that supports a strong, healthy foundation for the smile you want to share with the world.
-

 General2 months ago
General2 months agoWhat Is Felixing? The Truth Behind a Junk Keyword
-
 Health9 months ago
Health9 months agoLufanest: Effective Local Anesthesia with Fewer Risks
-

 Entertainment2 months ago
Entertainment2 months agoهنتاوي.com: Your Gateway to Arabic Anime Content
-

 General10 months ago
General10 months agobardoek: The Artistic Heritage Inspiring Modern Creative Trends
-

 General9 months ago
General9 months agoDiscover Anonib AZN: An Anonymous Asian Forum
-

 Fashion2 months ago
Fashion2 months agoFashionisk .com Explained: A Closer Look Before You Click
-

 Technology10 months ago
Technology10 months agoAponeyrvsh: A Modern Framework for Innovation and Resource Use
-

 Lifestyle10 months ago
Lifestyle10 months agoMariano Iduba: A Visionary Leader in Global Digital Growth





